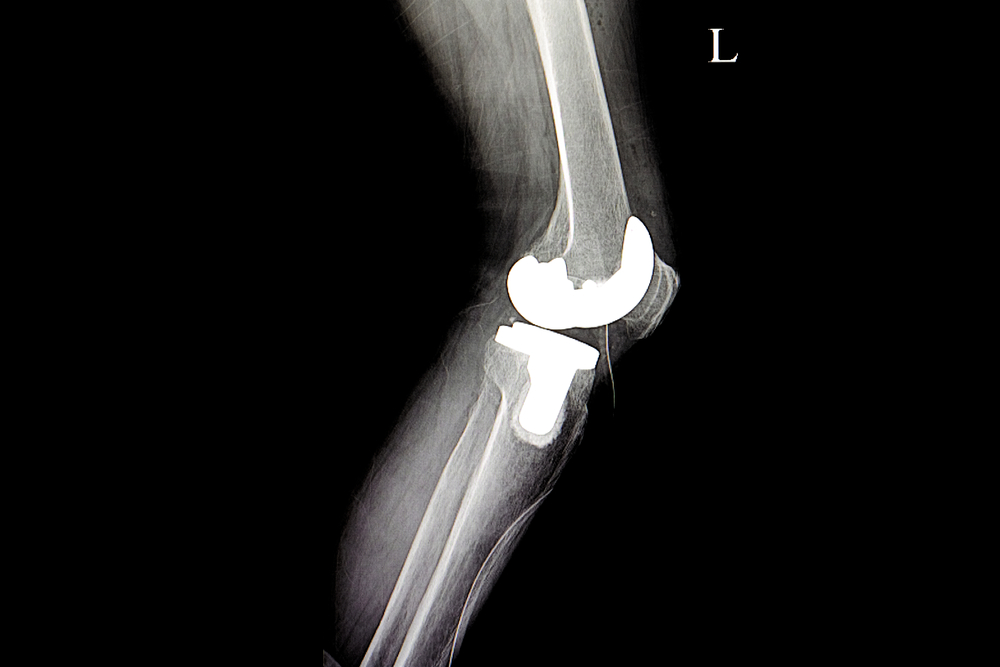
Should I Be Concerned About My Knees Getting So Bad That I Need a Knee Replacement?
In the quiet ache of a morning walk or the sharp twinge during a simple squat, many of us have felt the first whispers of knee trouble. As we age, our joints bear the cumulative toll of years—decades, even—of carrying us forward. For me, or perhaps for you reading this, that nagging discomfort in the knees isn’t just an annoyance; it’s a harbinger. Osteoarthritis (OA), the most common form of arthritis affecting the knees, strikes over 500 million people worldwide, with knee OA accounting for nearly 80% of the global burden. In the United States alone, millions grapple with this degenerative condition, and projections show its prevalence rising sharply due to aging populations and lifestyle factors like obesity. The question looms: Should I be concerned that my knees could deteriorate to the point of requiring total knee replacement surgery? The answer is a measured yes—concern is warranted, not as a paralyzing fear, but as a catalyst for informed action. While knee replacements are increasingly common and effective, they represent an end-stage intervention. By understanding the risks, recognizing warning signs, weighing the procedure’s realities, and embracing preventive strategies, we can often delay or even avoid the operating table. This essay explores these facets, urging a proactive stance toward joint health in an era where our mobility defines our independence.
Knee deterioration, primarily driven by osteoarthritis, is a slow-burning process where the protective cartilage cushioning the joint erodes, leading to bone-on-bone friction, inflammation, and pain. The pathogenesis involves a complex interplay of mechanical stress, inflammation, and genetic predispositions, but it’s the modifiable risk factors that demand our attention. Age is the most unyielding culprit: the incidence of knee OA surges after 50, with radiographic evidence appearing in up to 30% of those over 65. Women face a higher risk, possibly due to hormonal shifts post-menopause and wider pelvic structures that alter knee biomechanics. Obesity amplifies the threat exponentially; each pound of excess body weight exerts about four pounds of pressure on the knees during walking, accelerating cartilage breakdown. High body mass index (BMI) contributes to over 20% of OA cases globally, a modifiable factor that underscores the obesity epidemic’s role in joint demise.
Injuries compound the vulnerability. A history of knee trauma—such as anterior cruciate ligament (ACL) tears or meniscal damage—increases OA risk by three to six times, even decades later. Repetitive stress from occupations involving heavy lifting, kneeling, or prolonged standing, like farming or construction, further erodes joint integrity. Genetics play a subtler hand, with familial patterns suggesting inherited weaknesses in cartilage resilience. Emerging research also implicates metabolic factors, such as diabetes, which promotes inflammation, and even flatfoot deformities that misalign knee loading. In urban settings like Nanjing, China, studies reveal a knee OA prevalence of up to 40% in those over 50, linked to higher education (correlating with sedentary jobs) and elevated BMI. These factors aren’t isolated; they synergize. For instance, an overweight individual with a prior sports injury might see accelerated progression, turning a minor creak into chronic agony within years. Concern here is rational: ignoring these risks invites a future where stairs become mountains.
Yet, deterioration doesn’t announce itself dramatically; it creeps in with insidious symptoms that erode quality of life. Early knee OA might manifest as stiffness after inactivity, resolving with movement—a “gelling” phenomenon. As it advances, pain sharpens: dull aches during activity evolve into constant throbbing, even at rest, often worsening at night and disrupting sleep. Swelling from synovial inflammation creates a puffy, warm joint, while crepitus—grating sounds or sensations—signals crumbling cartilage. Functional decline follows: buckling knees during descent, reduced range of motion limiting deep squats, or an antalgic gait that favors the unaffected side, risking compensatory injuries elsewhere.
The tipping point for concern—and potential replacement—arrives when conservative measures falter. If pain persists despite six months of physical therapy, weight loss, and analgesics, and X-rays reveal significant joint space narrowing (indicating >50% cartilage loss), surgery enters the conversation. Daily activities become Herculean: grocery shopping triggers limping, or hobbies like gardening yield to couch confinement. Severe cases involve bone spurs (osteophytes) impinging nerves or visible deformities like varus (bow-legged) alignment. At this stage, the concern shifts from “should I worry?” to “how soon must I act?” Data from the UK’s National Joint Registry shows that delaying beyond two years of severe symptoms can complicate recovery. For those in their 50s or 60s, this isn’t just physical—it’s existential, as immobility hastens muscle atrophy and isolation.
Knee replacement, or total knee arthroplasty (TKA), offers a beacon of relief, but it’s no panacea. The procedure involves resurfacing the damaged joint with metal alloys and durable plastic, typically lasting 15-20 years. Success rates are impressive: over 90% of patients report substantial pain reduction and improved function at one year, with 82-85% of implants functioning well after 25 years. By 2025, advancements like robotic-assisted surgery have refined precision, reducing alignment errors and potentially extending implant life. Most patients regain 90-120 degrees of flexion, sufficient for driving or kneeling, and return to low-impact activities within three months.
However, complications temper optimism. Serious issues, like infections or blood clots, occur in under 2% of cases, but periprosthetic joint infections carry a grim 11.6% mortality risk over four years—higher than some cancers. Revision rates hover at 1.5% in the first year and 5-6% by five years, often due to loosening or wear. Recovery demands commitment: two weeks of inpatient rehab for some, plus ongoing therapy to combat stiffness. Not everyone qualifies; smokers, the morbidly obese, or those with active infections face higher risks. Thus, while TKA restores lives—over 800,000 annually in the U.S.—it’s a last resort, prompting valid concern about reaching that juncture.
The silver lining lies in prevention and management, transforming concern into empowerment. Foremost, maintain a healthy weight: shedding just 10 pounds can halve knee load during strides, slashing OA progression by 50%. Low-impact exercise—swimming, cycling, or tai chi—bolsters quadriceps and hamstrings, stabilizing the joint without undue stress. Physical therapy tailors strengthening routines, while braces or orthotics correct misalignments. Pharmacologically, acetaminophen or topical NSAIDs offer relief without GI risks, and intra-articular corticosteroid injections provide temporary respite for flares. Lifestyle tweaks matter: use ergonomic tools for repetitive tasks, wear supportive shoes, and protect knees during sports with proper warm-ups. Early intervention is key; studies affirm that addressing risk factors like obesity and injury history can prevent 14% of incident cases. For those already symptomatic, multidisciplinary care—combining dietitians, therapists, and rheumatologists—delays surgery by years.
Yes, be concerned about your knees veering toward replacement territory—it’s a prevalent, progressive foe fueled by controllable risks like weight and inactivity. Yet, this concern needn’t breed despair. Armed with knowledge of symptoms, surgical realities, and proven preventives, you hold the reins. Start today: track your pain, consult an orthopedist for imaging if stiffness lingers, and commit to movement that nourishes rather than punishes your joints. In a world where longevity outpaces vitality, safeguarding your knees isn’t optional—it’s the stride toward a fuller life. Remember, while statistics paint a sobering picture, individual outcomes hinge on action. Your knees have carried you this far; now, carry them wisely into tomorrow.